Ibrutinib improves survival for younger people with diffuse large B-cell lymphoma
Thursday, November 4, 2021
Ibrutinib improves survival for younger people with diffuse large B-cell lymphoma
New evidence suggests that adding the targeted therapy ibrutinib (Imbruvica) to a standard chemotherapy regimen can improve how long some younger people with a specific form of diffuse large B-cell lymphoma (DLBCL) live. The findings, published Nov. 4, 2021, in Cancer Cell, come from a new analysis by researchers at the National Cancer Institute (NCI), part of the National Institutes of Health, of a previously conducted phase 3 clinical trial.
Initial results from that study, known as the PHOENIX trial, showed that combining ibrutinib with the standard chemotherapy regimen did not help patients with a form of DLBCL called non-GCB DLBCL to live longer overall. However, by analyzing tumor biopsy samples from patients on the trial, NCI researchers and their collaborators have now shown that younger patients with specific genetic subtypes of non-GCB DLBCL, called MCD and N1, had an exceptional response to the treatment combination, with all such patients alive without disease three years after diagnosis.
“People thought the trial didn’t work,” said Louis M. Staudt, M.D., Ph.D., chief of the Lymphoid Malignancies Branch in the Cancer for Cancer Research at NCI. “But there was something interesting going on — if you just considered younger patients under the age of 60, they had a real benefit from ibrutinib, and we now understand why.”
“This new analysis provides a compelling rationale for doctors to consider adding ibrutinib to standard chemotherapy for the initial treatment of younger patients with non-GCB DLBCL,” said Wyndham H. Wilson, M.D., Ph.D., senior investigator in the Lymphoid Malignancies Branch and a co-author of the study.DLBCL is the most common type of lymphoma, accounting for 40% of lymphoma cases worldwide. This fast-growing cancer affects B cells, a type of white blood cell, and usually starts in the lymph nodes. People with DLBCL are typically treated with a chemotherapy regimen known as R-CHOP that includes cyclophosphamide, doxorubicin, vincristine, prednisone, and the monoclonal antibody rituximab. But R-CHOP is not effective for all people with DLBCL.
In the 2000s, to better understand individual variation in treatment response, researchers analyzed the patterns of gene activity in DLBCL tumors. They discovered that there are three molecular subgroups of DLBCL: germinal center B cell–like (GCB), activated B cell–like (ABC), and unclassified. Researchers later found that these subgroups respond differently to chemotherapy. More recently, researchers showed that the ABC and GCB subgroups can be further divided into seven genetic subtypes that also respond differently to chemotherapy.
Ibrutinib was the first targeted therapy to be evaluated for the treatment of DLBCL. The drug works by blocking the activity of Bruton tyrosine kinase, a protein that is involved in the growth and survival of B cells. Cancer cells of ABC DLBCL require this protein to survive. In a previous phase 2 clinical trial involving patients with relapsed DLBCL, researchers found that treatment with ibrutinib alone resulted in tumor shrinkage in 37% of patients with the ABC type but only 5% of those with the GCB type.
Subsequently, researchers launched the PHOENIX trial to evaluate the impact of adding ibrutinib to R-CHOP in patients with newly diagnosed non-GCB DLBCL. Although that trial showed no survival benefit of adding ibrutinib to R-CHOP overall, when the researchers looked specifically at trial participants aged 60 and younger, the benefits of adding ibrutinib to R-CHOP became evident. Patients older than age 60 did not benefit from the addition of ibrutinib to R-CHOP, likely because they frequently did not tolerate this combination well and had to stop treatment early.
What was unclear from the PHOENIX trial was whether all younger patients with non-GCB DLBCL benefited from ibrutinib, or if there was greater benefit for patients with certain genetic subtypes. To gain insights into this question, researchers performed genetic analyses on tumor samples from 773 of the 838 participants and determined their subtypes using an algorithm called LymphGen that Dr. Staudt developed with his NCI colleague George Wright, Ph.D.
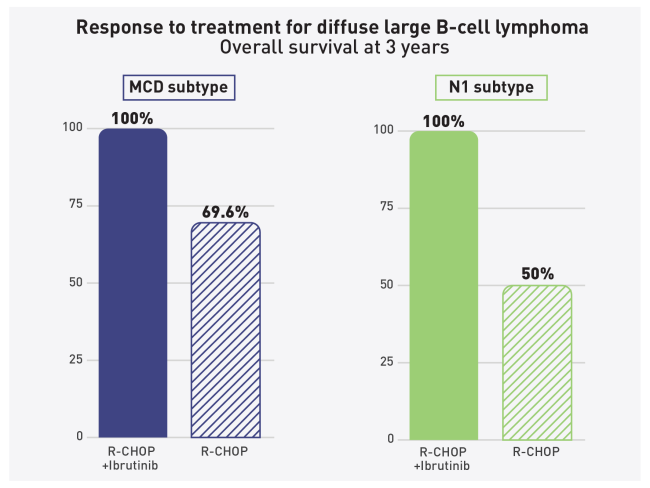
They showed that most of the benefit from ibrutinib was in patients with ABC DLBCL, mirroring the previous study. ABC DLBCL can be divided into four genetic subtypes: MCD, N1, BN2, and A53. The researchers found that patients who were 60 and younger with the MCD subtype had three-year event-free and overall survival rates of 100% with ibrutinib and R-CHOP, compared with three-year event-free survival of 48% and three-year overall survival of 69.6% with R-CHOP alone. Younger patients with the N1 subtype also had three-year event-free and overall survival rates of 100% with ibrutinib and R-CHOP, compared with three-year event-free and overall survival of 50% with R-CHOP alone.
Younger patients with the BN2 genetic subtype did not appear to benefit from the addition of ibrutinib. However, that subtype already had an 82% overall survival rate with R-CHOP alone.
In addition to the exceptional response rate in MCD and N1 DLBCL, ibrutinib did provide benefit for some other younger patients with non-GCB DLBCL. More research is needed to determine whether the A53 subtype — which the researchers could not identify in this study because of technical reasons — falls into this category.
Although no tests are commercially available to identify the MCD and N1 subtypes, Dr. Staudt pointed out that the identification of non-GCB DLBCL is done routinely.
“For years we have only had chemotherapy and rituximab to offer these patients,” he said. “Now, we hope that adding ibrutinib to current therapy may give younger patients a better chance of surviving this aggressive cancer.”
This study was supported by the Intramural Research Programs of NIH and NCI. Janssen Research and Development, LLC, sponsored the PHOENIX trial.
About the Center for Cancer Research (CCR): CCR comprises nearly 250 teams conducting basic, translational, and clinical research in the NCI intramural program—an environment supporting innovative science aimed at improving human health. CCR’s clinical program is housed at the NIH Clinical Center—the world’s largest hospital dedicated to clinical research. For more information about CCR and its programs, visit ccr.cancer.gov.
About the National Cancer Institute (NCI): NCI leads the National Cancer Program and NIH’s efforts to dramatically reduce the prevalence of cancer and improve the lives of cancer patients and their families, through research into prevention and cancer biology, the development of new interventions, and the training and mentoring of new researchers. For more information about cancer, please visit the NCI website at cancer.gov or call NCI’s contact center, the Cancer Information Service, at 1-800-4-CANCER (1-800-422-6237).
About the National Institutes of Health (NIH): NIH, the nation's medical research agency, includes 27 Institutes and Centers and is a component of the U.S. Department of Health and Human Services. NIH is the primary federal agency conducting and supporting basic, clinical, and translational medical research, and is investigating the causes, treatments, and cures for both common and rare diseases. For more information about NIH and its programs, visit www.nih.gov.
NIH…Turning Discovery Into Health®
Wilson WH, Wright G, Huang DA, et al. Effect of ibrutinib with R-CHOP chemotherapy in genetic subtypes of DLBCL. Cancer Cell November 4, 2021. DOI: 10.1016/j.ccell.2021.10.006.
Institute/Center
Contact
240-760-6600


