High blood pressure awareness and treatment declining
September 22, 2020
High blood pressure awareness and treatment declining
At a Glance
- After increasing between 1999 and 2014, both awareness and treatment of high blood pressure dropped among adults in the U.S.
- Efforts to identify and treat more people with high blood pressure could reduce the number of strokes and other serious health problems caused by the condition.
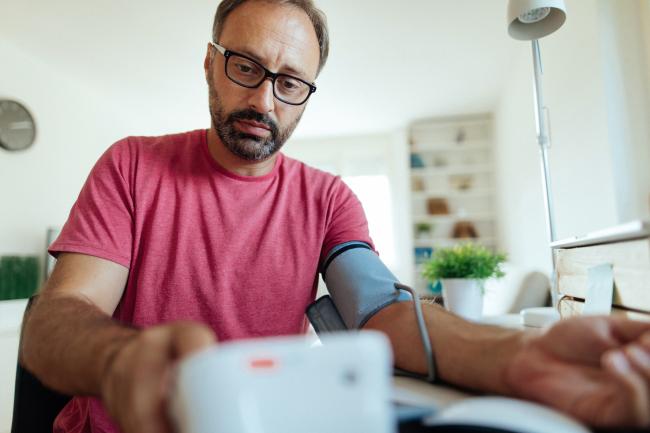
Nearly half of adults in the U.S. live with high blood pressure, also called hypertension. It is currently defined as having a blood pressure reading of at least 130/80 mm Hg or taking blood pressure medications for the condition. High blood pressure is the main risk factor for stroke. It can also contribute to other serious health problems, including chronic kidney disease, heart attack, and heart failure.
Most people can control high blood pressure with lifestyle changes, medications, or a combination of both. But many adults don’t even know they have the condition. They often don’t have symptoms before it has caused damage.
Both awareness and treatment of high blood pressure started rising around the turn of the century. Researchers led by Dr. Paul Muntner from the University of Alabama at Birmingham looked into whether that increase was sustained. To examine recent trends in high blood pressure, they used data from a large national health survey. The survey is conducted every two years using a representative sample of Americans.
The team compared the number of people with hypertension from 10 cycles of the survey, from 1999 through 2018. At the time, hypertension was defined by a blood pressure reading of 140/90 mm Hg or higher. The team also looked at how many people with the condition knew they had it and how many were receiving treatment.
The study was funded in part by NIH’s National Heart, Lung, and Blood Institute (NHLBI). Results were published on September 9, 2020, in JAMA.
Out of more than 50,000 adults surveyed between 1999-2018, over 18,000 had high blood pressure. The percentage of people who had the condition rose from 30% in 1999 to 32% in 2017.
The number of those with hypertension who had their blood pressure under control rose from about 32% in 1999-2000 to almost 54% in 2013-2014. However, by 2017-2018 that number had dropped to just under 44%.
Awareness of high blood pressure also increased from about 70% of adults with hypertension in 1999-2000 to almost 85% in 2013-2014. But it then dropped to 77% by 2017-2018.
Adults aged 46-64 were more likely to have their blood pressure controlled than both younger adults and people aged 75 and older. Black adults were less likely than white adults to have controlled high blood pressure. People with health insurance and a usual health care provider were more likely to have control over their high blood pressure than those without health insurance or regular contact with the health care system.
“The reversal in hypertension awareness is a real setback in the fight to reduce heart disease and stroke,” Muntner says. “While lifestyle factors are big contributors to hypertension, awareness and appropriate treatment are key to lowering blood pressure and keeping it in a healthy range to greatly reduce the risk for heart disease and stroke.”
Greater efforts are needed to increase screening for high blood pressure, particularly among younger adults, and support adherence to treatment.
Related Links
- Intensive Blood Pressure Control May Lessen Cognitive Loss
- Wearable Ultrasound Patch Tracks Blood Pressure
- The Genetics of Blood Pressure
- Blood Pressure Management for Seniors
- Comparing Blood Pressure Control Targets
- Program Improves Blood Pressure Control
- Blood Pressure Matters
- High Blood Pressure (Hypertension)
- National Health and Nutrition Examination Survey: NHANES (CDC)
References
Trends in Blood Pressure Control Among US Adults With Hypertension, 1999-2000 to 2017-2018. Muntner P, Hardy ST, Fine LJ, Jaeger BC, Wozniak G, Levitan EB, Colantonio LD. JAMA. 2020 Sep 9. doi: 10.1001/jama.2020.14545. Online ahead of print. PMID: 32902588.Obesity and Hypertension in the Time of COVID-19. Rodgers GP, Gibbons GH. JAMA. 2020 Sep 9. doi: 10.1001/jama.2020.16753. Online ahead of print. PMID: 32902581.


