Treating newborns with opioid withdrawal
May 12, 2026
Treating newborns with opioid withdrawal
At a Glance
- A clinical trial showed that giving opioid withdrawal medications based on an infant’s symptoms rather than a set schedule can shorten hospital stays.
- The findings suggest that as-needed treatment for infant withdrawal may lower the risk of over-treatment.
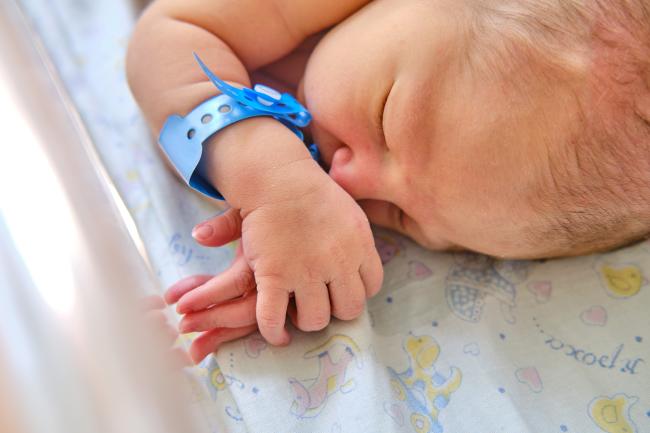
Opioid use during pregnancy may lead to opioid withdrawal in the baby after delivery. This condition is known as neonatal opioid withdrawal syndrome (NOWS). Experts have long debated the best way to treat these infants.
Two different methods are generally used to assess infants’ symptoms. The historical Finnegan approach uses a score based on a list of 21 withdrawal symptoms. However, recent studies suggest that better outcomes result from using a newer method called Eat, Sleep, Console (ESC). ESC focuses on an infant’s ability to eat, sleep, and be consoled.
With either approach, once medications begin, hospitals historically have treated NOWS using a scheduled opioid taper. Doctors give scheduled doses of opioid medication to control symptoms, progressively lowering the dose to wean babies off. A newer approach, called symptom-based dosing, allows doctors to give doses on an “as needed” basis. This may reduce the need for unnecessary medications. However, no studies have been done to compare the two approaches and determine which was better.
An NIH-funded clinical trial, led by Dr. Lori Devlin at the University of Louisville and Dr. Leslie Young at the University of Vermont, compared symptom-based dosing with scheduled dosing at 23 U.S. hospitals. Of these hospitals, 15 used ESC and 8 used the Finnegan approach. A total of 383 infants were assessed with ESC and included in the study’s main analysis. Results of the study were published in JAMA on April 25, 2026.
Among infants evaluated with the ESC approach, those in the symptom-based dosing group were ready to be discharged from the hospital nearly two and a half days sooner on average than infants in the scheduled dosing group. They also received fewer doses of opioids. The symptom-based dosing was adequate for about two-thirds of the infants treated with the approach. These infants avoided a long medication taper. The remaining infants had to switch to scheduled dosing to adequately treat their symptoms.
The findings suggest that symptom-based dosing better helps to match the amount of medication used with the severity of withdrawal. In addition, symptom-based dosing was as safe as a scheduled opioid taper, based on infant outcomes up to three months of age.
These results show that treating NOWS with ESC and symptom-based dosing can shorten the length of hospital stay. It can also reduce the amount of medication used.
“The opioid epidemic is still a huge problem, but this is a simple and powerful way we can get these babies ready to go home faster,” says Dr. Augusto Schmidt, a co-author of the study and a program officer at NIH’s Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD). “This is best for their family and for their own development.”
—by Brandon Levy
Related Links
- High-dose buprenorphine for opioid withdrawal
- Telehealth improves treatment for opioid use disorder
- Opioid overdose deaths rise among Black Americans
- Opioid facts for parents
- About opioid use during pregnancy
- Treat and manage infants affected by prenatal opioid exposure
References
Symptom-Based Dosing for Neonatal Opioid Withdrawal: The OPTimize NOW Randomized Clinical Trial. Devlin LA, Babineau DC, Merhar SL, DeMauro SB, Kraft WK, Lorch SA, Das A, McDonald SA, Rhodes E, Schmidt AF, Trochinski L, Crawford M, Sithisarn T, Leeman L, Kovatis KZ, Ambalavanan N, Smith RW, Telang S, Tioseco JA, McAllister JM, Wexelblatt SL, Muniyappa B, Williams PK, Adeniyi-Jones SC, Hill CD, Wright T, Sokol GM, Johnson L, Hall RW, Duncan SD, Puopolo K, Dummula K, Anderson-Berry A, Davis JM, Poindexter B, Young LW; HEAL Evaluation of Limited Pharmacotherapies for Neonatal Opioid Withdrawal Syndrome (HELP for NOWS) Consortium. JAMA. 2026 Apr 25:e265782. doi: 10.1001/jama.2026.5782. Epub ahead of print. PMID: 42033722.
Funding
NIH Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD).


