You are here
December 7, 2017
Testimony on the Implementation of the 21st Century Cures Act: Progress and the Path Forward for Medical Innovation
Witness appearing before the Senate Committee on Health, Education, Labor, and Pensions
Francis S. Collins, M.D., Ph.D.
Director, National Institutes of Health
Chairman Alexander, Ranking Member Murray, and Distinguished Members of this Committee, thank you for hosting this important hearing.
More so, thank you for creating the need for this hearing – for the 21st Century Cures Act (Cures Act) which was enacted one year ago. The Cures Act touches on so many important issues. From providing support for four cutting edge research priorities, to enhancing privacy protections to inclusion of various communities in research trials, to reducing administrative burden to expanded prize authority, we at NIH appreciate your leadership and dedication in enacting new authorities to speed the pace of research and improve how science is conducted to transform the way we translate discovery into therapies.
In my testimony, I will highlight how NIH is implementing some of the key provisions of the Cures Act and how it is benefiting the biomedical research community and, most importantly, patients.
Big Data: The Promise of Data Sharing Balanced With the Need for Privacy
As in most fields, computing power is changing the way research is done. The promise of big data cannot be overstated for finding patterns of disease and health and targeting therapeutics to sub-populations. The Congress, in the Cures Act, wisely recognized both the potential and the risks inherent in sharing data sets and NIH has moved quickly to get the appropriate protections in place.
First, on September 7th, NIH issued a Guide Notice to our research community implementing the significant enhancements this Committee made to the Certificates of Confidentiality, making them both automatic and compulsory. To implement this change while minimizing the burden to our researchers, we streamlined the issuance of Certificates into the terms and conditions of every research award we make involving human subjects.1 Since October 1st, every NIH award has this added layer of protection for research participants.
Second, on September 17th, guidance on the FOIA exemption for genomic information was disseminated to all NIH FOIA officers.
Only now that the new Cures Act privacy protections are in place, are we moving forward on the exciting new authority to require data sharing. This will be a sea change in biomedical research so we must be deliberate about how to measure the usefulness of data sets, where shared data should be stored, how patient protections are insured, how interoperability is achieved, and what tools researchers most need in the shared environment. On November 6th, NIH made 12 awards in a Data Commons Pilot to answer just these kind of questions. We selected three prominent NIH datasets researchers can use to test their processes. The biomedical research community will be watching this pilot program very closely.
Inclusion
We’ve made tremendous progress in managing diseases through the development of new drugs and devices over the years that were tested in clinical trials. But trials haven’t always included the full spectrum of humanity, and this limits the applicability of study results. It also limits our ability to target therapies and address disparities. Congress helped NIH address this issue through the Cures Act in three focus areas: inclusion of children and seniors; inclusion of pregnant and lactating women; and continuing our focus on women, and racial and ethnic minorities.
On June 1-2, 2017, as required by the Cures Act, NIH held a workshop on inclusion across the lifespan. It might seem easy to include all age ranges but both children and older adults require special considerations. At the workshop, investigators with expertise in conducting clinical studies with pediatric and older populations, ethics experts, and other stakeholders had a robust discussion about barriers and facilitators to the inclusion of volunteers of all ages in research. The findings and recommendations will be presented at my Advisory Committee meeting on December 14-15, 2017, and we will determine what policy changes are needed to ensure individuals across the lifespan are appropriately included in clinical research.
The Cures Act also asks NIH to continue making progress on the inclusion of women and ethnic and racial minority populations in research. This has been a partnership of the Congress and NIH for many years – the Congress authorized both the NIH Office of Research on Women’s Health and what is now the National Institute on Minority Health and Health Disparities in 1993. With the help of the Congress and the Cures Act, we continue to improve. We are now collecting inclusion data on a study-by-study basis and in the coming year NIH will report, for the first time, inclusion data from studies on a disease and condition basis. At the December meeting, the expert Advisory Committee will have a public discussion of recommendations for further advancing the field and updating our inclusion guidelines. I look forward to the conversation and I will be happy to update you as decisions are made.
Finally, the Cures Act created a Task Force on Research Specific to Pregnant Women and Lactating Women (PRGLAC) to advise the Secretary of Health and Human Services regarding gaps in knowledge and research on safe and effective therapies for pregnant women and lactating women.2 This area of research is vital, but it is absolutely critical that we carefully consider intentional exposures in this potentially vulnerable time of life. NIH established PRGLAC on March 13, 2017, bringing together federal and non-federal experts, including the Food and Drug Administration, representatives from relevant medical societies, non-profit organizations, and industry, to discuss these important issues.
PRGLAC has already held two meetings – the first on August 21-22, 2017, to determine the scope of current Federal activities on safe and effective therapies for pregnant and lactating women, and the second on November 6-7, 2017, to understand the ethical issues surrounding research to develop therapies for pregnant and lactating women. The third meeting on February 26-27, 2018, will be on communication strategies for health care providers and the public about the use of therapies for pregnant and lactating women, and the fourth meeting on May 14-15, 2018, will be on recommendations to address the gaps in knowledge, ethical issues, and communication strategies for therapies used by pregnant and lactating women.
Based on the outcome of the Task Force meetings, a report with recommendations will be developed for the HHS Secretary. NIH is grateful to the Congress for recognizing the need for careful consideration in this area of research and looks forward to addressing any recommendations made by the Task Force.
Strengthening Biomedical Workforce
NIH and its stakeholder community have for many years been concerned about the long-term stability of the biomedical research enterprise. As a consequence of NIH’s loss of more than 20 percent of its purchasing power from 2003 to 2015, researchers were forced to vie for limited resources, leading to a hypercompetitive environment. With success rates below 20 percent, many highly meritorious applications continue to go unfunded. This has too often resulted in misaligned incentives and unintended consequences for talented researchers at all career stages who are trying to succeed and stay in science. The current environment is particularly challenging for many new- and mid-career investigators.
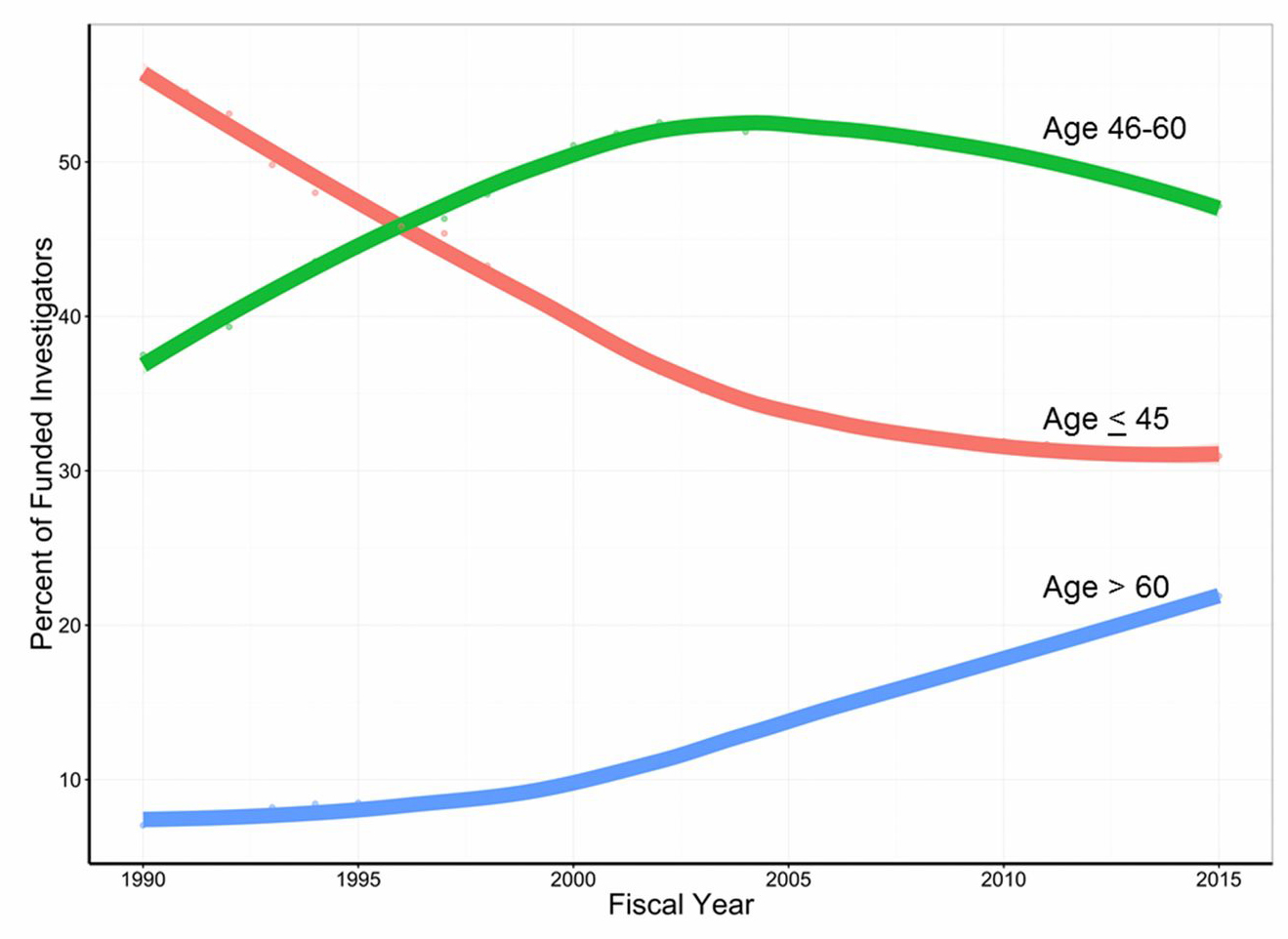
Over the last several years, NIH has taken numerous steps to balance, strengthen, and stabilize the biomedical research workforce, but these measures have only taken us so far. While the percentage of NIH awards that support early-career investigators has gone from declining to flat, these gains have been offset by a decline in the percentage of NIH awards that support mid-career investigators.
NIH will develop evidence-based, data-driven strategies to assure that NIH investments are directed in ways that maximize scientific output. Institutes and Centers will also place greater emphasis on current NIH funding programs to identify, grow, and retain new- and mid-career investigators across these critical career stages. The NIH Office of the Director will track progress across ICs and assess if these strategies are working. I am personally committed to this issue and thank the Committee for their support of early- and mid-career investigators.As a direct result of the Cures Act, in June 2017, NIH launched the Next Generation Researchers Initiative 3 aimed at strengthening the biomedical workforce with a focus on early career investigators or investigators who are at an early stage in their career. NIH intends to take a multi-pronged approach, which we outlined in an article published on November 7, 2017,4 to increase the number of NIH-funded early-stage and mid-career investigators and to stabilize the career trajectory of scientists.
System Innovation: Reducing Administrative Burden and Increasing Efficiency
Policies generated with the best intentions sometimes have serious adverse consequences for research. The Cures Act included numerous provisions that cut the bureaucratic red tape that slows the progress of science. It also provided NIH with new authorities to improve efficiencies and speed up the discovery process.
The Cures Act included provisions to improve ClinicalTrials.gov. ClinicalTrials.gov is a database of privately and publicly funded clinical studies conducted around the world that plays a crucial role in ensuring the transparency and accountability to the public of researchers and their sponsors. In addition, this resource is used by researchers to stay up-to-date on developments in their field, find collaborators, and identify unmet needs, and it is also used by patients and families to search for potential studies to enroll in or learn about new treatments that are being tested. NIH strives to make this resource as user friendly as possible so it can benefit researchers, patients, and their families, and the Cures Act is helping in several ways.
First, the Cures Act made technical fixes to the legislation establishing ClinicalTrials.gov that ensure NIH is able to capture more clinical trials in the system and improve our oversight and transparency. Second, it required NIH to consult with relevant Federal agencies and other stakeholders to receive recommendations to enhance ClinicalTrials.gov’s usability, functionality, and search capability. In February 2017, the National Library of Medicine (NLM), along with 18F, a digital services consultancy within the General Services Administration, began conducting user research on ClinicalTrials.gov with a range of stakeholders. As a result of this work, NIH rolled out a first in a series of changes to ClinicalTrials.gov on June 19, 2017. On September 25, 2017, NLM released more updates as the next phase in its ongoing effort to enhance the functionality of the database. In response to the Cures Act, NLM will work continuously to make it easier for users to find and participate in clinical trials.
In an effort to improve efficiency, the Cures Act provided a new EUREKA prize authority and allowed NIH to use Other Transactions Authority (OTA) in two areas that need extra flexibility and collaboration: the Common Fund and the All of Us Research program, part of the NIH Precision Medicine Initiative.
The EUREKA prize authority is being implemented in three ways:
- On November 2nd, the National Institute on Aging issued a request 5 for public input on (1) the feasibility of three potential prize competitions focused on Alzheimer’s disease (AD) and related dementias (ADRD): Validating predictors of AD progression; PET radiotracer to measure in vivo synaptic integrity; and low cost innovation of improving systems of care for AD/ADRD patients and caregivers; and (2) any other suggestions on AD/ADRD research goals to connect to a prize. Comments are due on December 31, 2017.
- NIH formed the EUREKA Prize Coordination Committee to review future proposals for future EUREKA prize competitions.
- NIH funded the National Academy of Sciences (NAS) to study Innovation Prizes and Federal R&D with specific emphasis on strategies to determine which “EUREKA” prize topics are consistent with congressional intent. The NAS study will also consider the strengths and weaknesses of various measures of health outcomes and effects on government expenditures. The NAS intends to hold a workshop in 2018.
OTA is integral to our exploration of how best to structure data sharing, known as the Data Commons Pilot Phase,6 which was announced on November 6th. The goal of the NIH Data Commons is to accelerate new biomedical discoveries by providing a cloud-based platform where investigators can store, share, access, and compute on digital objects (data, software, etc.) generated from biomedical research and perform novel scientific research including hypothesis generation, discovery, and validation. The use of OTA awards allows flexibility for the awardees to work together to design innovation solutions that meet the computational and scientific needs of the Pilot.
The All of Us Research Program aims to enroll one million individuals in a decades-long research project. That ambitious goal requires flexibility, complex and dynamic interactions, and ways to engage non-traditional NIH awardees to advance the mission. For example, All of Us has used OTA to make awards to the Healthcare Provider Organizations to help build the research protocols, test enrollment procedures, and collect essential health data and biological specimens.
The Cures Act also recognizes that two of the cornerstones of scientific advancement are rigor in designing and performing scientific research and the ability to reproduce biomedical research findings. In recent years, the scientific community has become aware of the need to improve rigor and reproducibility. In 2014, NIH worked with scientific publishers to develop a set of principles and goals that 79 publishers have now endorsed. As the Cures Act requires, my Advisory Committee has convened a Working Group on Rigor and Reproducibility and they are reviewing the experience of the last few years, leading to the development of recommendations for a formal policy. I look forward to updating you as this effort takes shape.
NIH Innovation Fund
Last, but certainly not least, the Cures Act provided multi-year funding through the NIH Innovation Fund for four highly innovative scientific research initiatives: the Precision Medicine Initiative (PMI), the Brain Research through Advancing Innovative Neurotechnologies® (BRAIN) Initiative, the Cancer Moonshot, and the Regenerative Medicine Innovation Project. As required by the Cures Act, on March 28th, I solicited recommendations from my Advisory Committee on how to allocate the funds. We had a robust conversation about each of the initiatives and the Advisory Committee members provided critical advice on how to move forward. As a result of that discussion, and conversations with my NIH colleagues, we drafted the NIH Innovation Fund Work Plan,7 which was submitted to Congress in September 2017, outlining how the agency will use the NIH Innovations Funds for each of these four initiatives. I would like to tell you a bit about each of these initiatives and how the NIH Innovation Funds are helping to move each initiative forward.
The Precision Medicine Initiative
Precision medicine is a revolutionary approach for disease prevention and treatment that takes into account individual differences in lifestyle, environment, and biology. While some advances in precision medicine have been made, the practice is not in use for most diseases. The All of Us Research Program, a key element of PMI, is building a national resource—one of the world's largest, most diverse biomedical data sets in history—to accelerate health research and medical breakthroughs, enabling individualized prevention, treatment, and care. All of Us will engage one million or more U.S. volunteers from all life stages, health statuses, races/ethnicities, and geographic regions to reflect the country’s diverse places and people to contribute their health data over many years to improve health outcomes, fuel the development of new treatments for disease, and catalyze a new era of evidence-based and more precise preventive care and medical treatment.
Across the nation, NIH has engaged 10 large health provider organizations, six community health centers, and the Veterans Administration to be our partners in this ambitious study. The program is launching in stages. The beta phase began in May 2017 during which each of our partners are testing their systems and processes to ensure a good experience for participants.
In July 2017, the program made its first four community partner awards to motivate diverse communities to join and remain in the program, with a focus on those traditionally underrepresented in biomedical research. Each of these organizations has deep, trusted relationships within and ties to their communities, and we are so very pleased to have the opportunity to partner with them to enhance our outreach into communities that have traditionally been underrepresented in biomedical research. NIH has also engaged with organizations to create mobile apps to enroll, obtain consent from, collect data from, and communicate with All of Us participants. One of our partners is working with FitBit on a pilot that will start in mid-2018 to test out ways for participants to easily and efficiently contribute data on physical activity, sleep, heart rates, and other behavioral health information.
We anticipate to roll out nationally in spring 2018. Following the national launch, we will make continuous improvements and updates to the program based on participant feedback and emerging scientific opportunities and technological advances. The Cures Act Innovation Funds will be critical to ensuring the success of All of Us and the promise of personalized medicine.
The BRAIN® Initiative
The BRAIN Initiative is aimed at revolutionizing our understanding of the human brain, the most complex structure in the known universe. Launched in 2013, this large-scale effort will push the boundaries of neuroscience research and equip scientists with insights necessary for treating a wide variety of brain disorders. By accelerating the development and application of innovative technologies, researchers will be able to produce a revolutionary new dynamic picture of the brain that, for the first time, shows how individual cells and complex neural circuits interact in both time and space. Long desired by researchers seeking new ways to treat, cure, and even prevent brain disorders, this picture will fill major gaps in our current knowledge and provide unprecedented opportunities for exploring exactly how the brain enables the human body to record, process, utilize, store, and retrieve vast quantities of information, all at the speed of thought.
NIH leveraged the Cures Act’s FY 2017 Innovation Funds, in addition to our annual appropriation, to launch 110 exciting new research projects.8 These projects are focused on developing detailed brain circuit maps and powerful new tools to monitor and modulate brain activity in animal models to benefit patients with neurological and psychiatric disorders. Understanding the way the brain processes information and how it lays down memories and retrieves them will be instrumental for understanding brain health, and ultimately, preventing brain disorders such as Alzheimer’s disease, Parkinson’s, schizophrenia, autism, drug addiction, and traumatic brain injury. These awards add to work already underway to give us a high-resolution picture of the circuits and networks in the brain, how they work, and where they can go wrong.
The Cancer Moonshot℠
The Cancer Moonshot,9 funded in the Cures Act, has an ambitious goal: to dramatically speed advances in cancer prevention, diagnosis, treatment, and care. The National Cancer Institute (NCI) solicited direct input from the public and convened a Blue Ribbon Panel (BRP) of the nation’s top cancer researchers, oncologists, patient advocates, and private-sector leaders. In September 2016, the BRP presented its report outlining ten ambitious and achievable recommendations to the NCI’s National Cancer Advisory Board. These recommendations shape the scientific blueprint of the Cancer Moonshot representing areas of research that are poised to accelerate our understanding of cancer and bring benefit to patients. Overall, the recommendations create a vision for future cancer research and treatment in which:
- Researchers can identify possible targets for the development of new cancer treatments and preventive interventions, including immunotherapy and immunoprevention, and learn more about how to avoid or overcome cancer drug resistance in patients;
- Diverse groups of patients contribute information about their cancer, obtain a genomic profile, learn what treatments might work best given their profile, and identify clinical trials that may be appropriate for them;
- Infrastructures are established so that health care providers and researchers can share, access, and analyze information that improves the understanding of how tumors evolve, better predicts treatment outcomes, and helps control patient symptoms and side effects.
Some of these goals are scientific in nature, and some are systemic. If we are to speed advances, we cannot simply do more of the same. We must transform the way we conduct research, the way we share results, and the way we get discoveries into patient care. In FY 2017, NIH made 142 Cancer Moonshot awards, including efforts to leverage advances in immunotherapy, understand drug resistance, and develop of new technologies to characterize tumors and test therapies. These national and international collaborations will drive discovery for cancer patients and their families. I would like to highlight one of those collaborations for you today.
On October 12, 2017, NIH and 11 leading biopharmaceutical companies launched the Partnership for Accelerating Cancer Therapies (PACT), a five-year public-private research collaboration totaling $215 million as part of the Cancer Moonshot.10 PACT will initially focus on efforts to identify, develop, and validate robust biomarkers — standardized biological markers of disease and treatment response — to advance new immunotherapy treatments that harness the immune system to attack cancer. We have seen dramatic responses from immunotherapy, often eradicating cancer completely for some cancer patients. We need to bring that kind of success — and hope — to more people with more types of cancers, and we need to do it quickly. A systematic approach like PACT will help us to achieve success faster.
With the support of the Congress, the Cancer Moonshot will transform the way cancer research is conducted and ensure that substantial progress is made for patients and their families.
The Regenerative Medicine Innovation Project
Regenerative medicine is an emerging area of science that holds great promise for treating and possibly even curing a variety of injuries and diseases. Regenerative medicine includes using stem cells and other technologies, such as engineered biomaterials and gene editing — to repair or replace damaged cells, tissues, or organs. Stem cell-based approaches are under development in labs around the world, and some have already moved into clinical trials. Such progress notwithstanding, much work remains to be done toward the development of safe and effective regenerative medicine interventions to realize the full potential of this field.
As a result of the Cures Act, NIH launched the Regenerative Medicine Innovation Project to support clinical research on adult stem cells while promoting the highest standards for carrying out scientific research and protecting patient safety. The $2 million Cures provided for this initiative in FY 2017 were amplified through matching funds and NIH Institute contributions to reach a total of just under $5 million. In September, NIH made eight clinical research awards 11 that cover a broad spectrum of science and new technologies, and have the potential to advance understanding and treatment of common diseases – including diabetes, anemia, corneal and other eye diseases, and chronic skin ulcers – as well as rare diseases, including idiopathic pulmonary fibrosis, inherited skin diseases, and sickle cell disease.
Several awards will explore the use of adult stem cells to make specialized cells and tissues that could help reduce the need for whole organ transplants or otherwise restore normal function. Others aim to develop reliable methods of generating red blood cells and platelets in the lab to improve the safety and supply of blood available for transfusion.
NIH looks forward to the opportunity the Cures Act provides to advance this field of science and is hosting a workshop on December 6-7, 2017,12 to explore the state of regenerative medicine science involving adult stem cells, with a focus on approaches for the development of safe and effective products. This will help inform our funding decisions in future fiscal years.
Conclusion
Thank you for your leadership and dedication that resulted in enacting the Cures Act one year ago. Over the past year, the Cures Act has provided NIH with critical resources and tools to advance our mission – to seek fundamental knowledge about the nature and behavior of living systems and the application of that knowledge to enhance health, lengthen life, and reduce illness and disability. We appreciate Congress’s support for NIH through the Cures Act and will continue to implement the law to accelerate scientific discoveries and benefit patients.
1 https://humansubjects.nih.gov/coc/index.
2 https://www.nichd.nih.gov/about/advisory/PRGLAC/Pages/index.aspx.
3https://grants.nih.gov/ngri.htm.
4 Michael Lauer, Lawrence Tabak, and Francis Collins, “Opinion: The Next Generation Researchers Initiative at NIH,” PNAS, 114 (2017): 11801-11803.
5 https://grants.nih.gov/grants/guide/notice-files/NOT-AG-17-018.html.
6 https://commonfund.nih.gov/bd2k/commons/awardees
7 https://www.nih.gov/sites/default/files/research-training/initiatives/nih-cures-innovation-plan.pdf.
8 https://www.braininitiative.nih.gov/funding/fundedAwards.htm.
9 https://www.cancer.gov/research/key-initiatives/moonshot-cancer-initiative.
11 https://www.nih.gov/rmi/fy-2017-funded-awards.
12 https://www.nih.gov/research-training/medical-research-initiatives/cures.
This page last reviewed on December 7, 2017