Early results show benefit of remdesivir for COVID-19
June 2, 2020
Early results show benefit of remdesivir for COVID-19
At a Glance
- Early results showed that remdesivir benefited hospitalized patients with severe COVID-19 who required supplemental oxygen.
- While the findings support remdesivir as a standard therapy for such patients, they suggest more research is needed to improve outcomes for people with COVID-19.
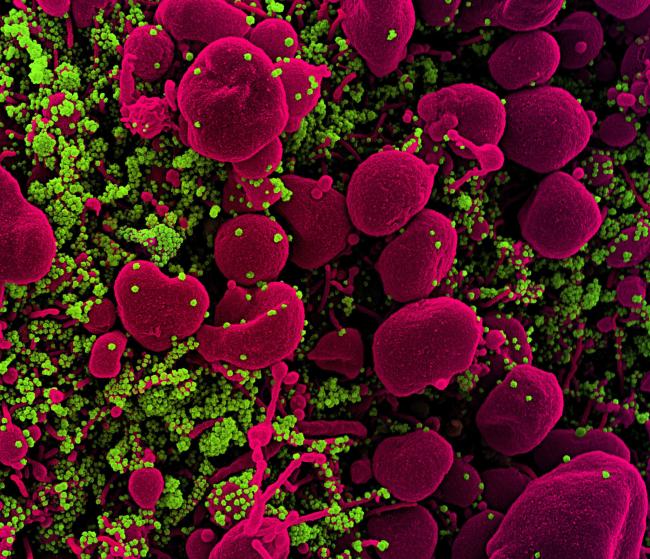
Coronaviruses are a large family of viruses that usually cause mild to moderate upper-respiratory tract illnesses like the common cold. SARS-CoV-2, the virus that causes coronavirus disease 2019 (COVID-19), is the third novel coronavirus to emerge over the past two decades. Since first appearing in China, COVID-19 has become an ongoing global pandemic. Infections can cause mild to extremely severe respiratory illness. Symptoms commonly include fever, cough, and shortness of breath.
By looking at studies on the previous two coronavirus outbreaks, which caused severe acute respiratory syndrome (SARS) and Middle East respiratory syndrome (MERS), researchers quickly identified potential treatments that might help reduce the severity of COVID-19. Remdesivir is one such investigational broad-spectrum antiviral treatment. It was previously tested in humans with Ebola virus disease and has shown promise in animal models for treating MERS and SARS.
To test whether remdesivir could help treat patients with COVID-19, a team of researchers carried out a randomized, controlled clinical trial called the Adaptive COVID-19 Treatment Trial (ACTT). The study enrolled 1,063 hospitalized adults with moderate to severe COVID-19 disease from across 10 countries over 58 days. The trial was funded by NIH’s National Institute of Allergy and Infectious Diseases (NIAID).
Patients were randomly assigned to receive a 10-day course of either remdesivir or an inactive placebo intravenously along with standard care. The trial was double-blind, meaning neither investigators nor participants knew who was receiving remdesivir or placebo. Although the study is still ongoing, an independent data and safety monitoring board overseeing the trial reviewed the data and shared their preliminary analysis with NIAID. Due to the public health implications, NIAID made these primary results public, and they were published on May 22, 2020, in the New England Journal of Medicine.
The analysis found that remdesivir shortened the time to recovery, which was defined as being medically stable enough to be discharged from the hospital. The median time to recovery was 11 days for patients treated with the drug compared with 15 days for those who received the placebo.
The results also suggest that the drug may have some benefit for surviving COVID-19. After 14 days, 7.1% of those in the group receiving remdesivir died versus 11.9% of those in placebo group. However, this difference was not large enough to prove that it wasn’t due to chance.
The researchers will continue to analyze the results after all the participants have completed 28 days of follow-up. That may provide additional insights into the treatment. NIAID has also begun a clinical trial (known as ACTT 2) to evaluate remdesivir in combination with the anti-inflammatory drug baricitinib.
“These results support the use of remdesivir for patients hospitalized with COVID-19 who require supplemental oxygen therapy. However, they also indicate the need to continue evaluating other therapeutic agents to further improve clinical outcomes for patients with COVID-19,” says NIAID Director Dr. Anthony S. Fauci.
Related Links
- Llama Antibody Engineered to Block Coronavirus
- Microneedle Coronavirus Vaccine Triggers Immune Response in Mice
- Novel Coronavirus Structure Reveals Targets for Vaccines and Treatments
- Study Suggests New Coronavirus May Remain on Surfaces for Days
- Coronaviruses
References
Remdesivir for the Treatment of Covid-19 - Preliminary Report. Beigel JH, Tomashek KM, Dodd LE, Mehta AK, Zingman BS, Kalil AC, Hohmann E, Chu HY, Luetkemeyer A, Kline S, Lopez de Castilla D, Finberg RW, Dierberg K, Tapson V, Hsieh L, Patterson TF, Paredes R, Sweeney DA, Short WR, Touloumi G, Lye DC, Ohmagari N, Oh MD, Ruiz-Palacios GM, Benfield T, Fätkenheuer G, Kortepeter MG, Atmar RL, Creech CB, Lundgren J, Babiker AG, Pett S, Neaton JD, Burgess TH, Bonnett T, Green M, Makowski M, Osinusi A, Nayak S, Lane HC; ACTT-1 Study Group Members. N Engl J Med. 2020 May 22. doi: 10.1056/NEJMoa2007764. Online ahead of print. PMID: 32445440.
Funding
NIH’s National Institute of Allergy and Infectious Diseases (NIAID) and National Cancer Institute (NCI); U.S. Department of Defense; the governments of Japan, Mexico, Denmark, and Singapore; Seoul National University Hospital; United Kingdom Medical Research Council.


