You are here
January 30, 2018
Altered lung structure may increase COPD risk
At a Glance
- A study found a link between variations in the structure of the lung’s airways and the risk of developing chronic obstructive pulmonary disorder (COPD).
- The findings suggest that chest CT scans can be used to identify people who have a higher risk for developing COPD.

Chronic obstructive pulmonary disease (COPD) is a serious lung disease that makes it hard to breathe. It’s a leading cause of death in the United States. Experts estimate that 16 million Americans have COPD. A constant cough, shortness of breath, and wheezing are symptoms. Smoking is an important risk factor for COPD, but nonsmokers can develop the disease, too. Finding other risk factors could help lead to better prevention and treatment strategies.
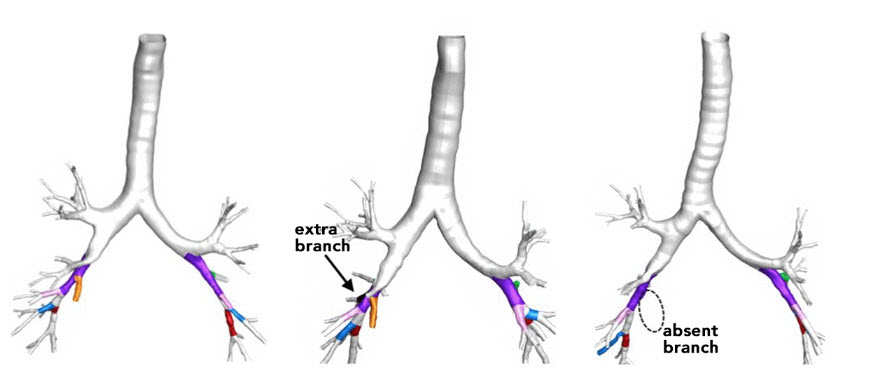
The airway tree of the lungs has many branches. The bronchial tubes branch many times into thousands of smaller, thinner tubes called bronchioles. These tubes end in bunches of tiny round air sacs called alveoli. Autopsy studies of diseased lungs have found that some people have variations from the standard branching pattern.
Dr. Benjamin M. Smith and colleagues at Columbia University Medical Center led a multisite study to investigate whether differences in airway branching patterns might play a role in susceptibility to COPD. The study was funded by NIH’s National Heart, Lung, and Blood Institute (NHLBI). Results appeared online on January 16, 2018, in the Proceedings of the National Academy of Sciences.
The researchers analyzed chest CT scans of more than 3,000 adults between 60 and 78 years old. More than half were current or former smokers. A substantial proportion of the airways (26.5%) varied from a standard branching pattern. More than 6% had a missing branch in the lower airway, 16% had an extra branch, and more than 4% had a combination of these variations or rarer patterns. By examining siblings, the scientists found that these patterns may run in families.
Next, the research team assessed whether any of the variants in branching patterns were associated with COPD. For this analysis, they included data from a second study that obtained CT scans from more than 1,800 people with COPD and more than 900 controls. They found that people with an extra branch were more likely than those with the standard branching pattern to develop COPD. For people with the missing branch from the lower airway, COPD risk was higher among smokers.
“In the current study, we found that central airway branches of the lungs, which are believed to form early in life, do not follow the textbook pattern in one quarter of the adult population, and these non-textbook variations in airway branches are associated with higher COPD prevalence among older adults,” Smith says. “Interestingly, one of the airway branch variants was associated with COPD among smokers and non-smokers. The other was associated with COPD, but only among smokers.”
Further study is needed to find out whether prevention or treatment interventions would improve health outcomes for people with an airway branching pattern variant.
Related Links
- Long-Term Oxygen For COPD
- Improved COPD Detection
- Out of Breath? Get Tested for COPD
- What Is COPD?
- COPD (Chronic Obstructive Pulmonary Disease)
- Bronchi, Bronchial Tree, and Lungs
References: Human airway branch variation and chronic obstructive pulmonary disease. Smith BM, Traboulsi H, Austin JHM, Manichaikul A, Hoffman EA, Bleecker ER, Cardoso WV, Cooper C, Couper DJ, Dashnaw SM, Guo J, Han MK, Hansel NN, Hughes EW, Jacobs DR Jr., Kanner RE, Kaufman JD, Kleerup E, Lin CL, Liu K, Lo Cascio CM, Martinez FJ, Nguyen JN, Prince MR, Rennard S, Rich SS, Simon L, Sun Y, Watson KE, Woodruff PG, Baglole CJ, Barr RG; MESA Lung and SPIROMICS investigators. Proc Natl Acad Sci U S A. 2018 Jan 16. pii: 201715564. doi: 10.1073/pnas.1715564115. [Epub ahead of print]. PMID: 29339516.
Funding: NIH’s National Heart, Lung, and Blood Institute (NHLBI); U.S. Environmental Protection Agency; McGill University Health Center Research Institute; and Fonds de la recherche en santé Québec (Quebec Health Research Fund).