Brain stimulation can affect memory in older adults
September 13, 2022
Brain stimulation can affect memory in older adults
At a Glance
- A noninvasive method that stimulates specific brain regions led to month-long memory improvements in older adults.
- The approach suggests the potential of using a noninvasive, drug-free treatment to reverse or prevent memory loss in the aging population.
The number of older adults worldwide is rising, along with an increase in age-related memory decline. Researchers have long sought ways to prevent or reverse memory impairment. They’ve been able to pinpoint specific brain circuits and networks that underlie learning and memory. But effective and lasting interventions to improve memory have remained elusive.
An NIH-funded research team at Boston University led by Dr. Robert Reinhart has been exploring noninvasive approaches to improve memory in aging populations. Based on earlier research, the scientists suspected that low-frequency stimulation to the parietal region near the back of the brain would improve short-term working memory, whereas high-frequency stimulation to the prefrontal cortex at the front of the brain would improve long-term memory.
They tested their hypothesis in a randomized, double-blinded study that included 150 volunteers, ages 65 to 88. They used a technique called high-definition transcranial alternating current stimulation (HD-tACS). The method involves applying weak electrical currents of particular frequencies to specific brain regions to help modify and synchronize the brain’s rhythmic activities. Results were reported in the September 2022 issue of Nature Neuroscience.
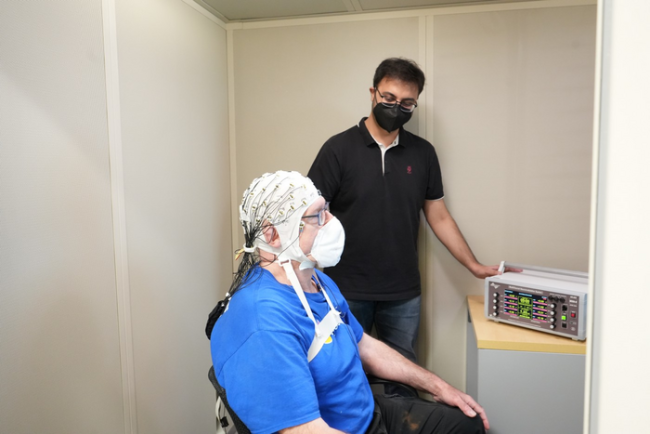
Participants received 20 minutes of stimulation or a sham treatment for three or four consecutive days. At the start of each session, they donned an electrode-studded skull cap that delivered currents to specific brain regions. The control group received a sham treatment of two 30-second pulses of stimulation, at the start and end of each session, to generate tingly sensations like those felt in the active treatment groups.
To assess memory during the treatment sessions, researchers read aloud five lists of 20 common words. At the end of each list, participants were asked to recall as many words as possible. More recently heard words at the end of the lists involved working memory. Words recalled near the beginning of the list needed to use long-term memory. Memory was also assessed at baseline (before treatments began) and 30 days later.
Participants who received low-frequency stimulation to the back of the brain had improved working memory on the third and fourth days of treatment as well as one month later. Those receiving high-frequency stimulation to the same brain region showed no such improvement.
In contrast, volunteers given high-frequency, but not low-frequency, stimulation to the front of the brain showed improved long-term memory on the second through fourth days of treatment and one month later.
The researchers found that the pace of memory improvement seen over the four days of treatment predicted memory strength one month later. And people who began the study with poorer cognitive function had greater and more enduring improvements. The findings suggest that the activity and functioning of the aging brain can be sustainably altered and improved by using noninvasive techniques to modify specific brain rhythms.
“Further research is needed to determine whether these effects can last beyond one month and whether these specific methods can also enhance memory function in individuals with impaired cognition due to brain disorders and in those at risk for dementia,” Reinhart says.
—by Vicki Contie
Related Links
- Some Brain Functions May Improve with Age
- Memories Involve Replay of Neural Firing Patterns
- A Noninvasive Deep Brain Stimulation Technique
- Recalling Temporary Memories
- A Well-Aged Mind
- Sleep On It
- Memory, Forgetfulness, and Aging: What's Normal and What's Not?
References
Long-lasting, dissociable improvements in working memory and long-term memory in older adults with repetitive neuromodulation. Grover S, Wen W, Viswanathan V, Gill CT, Reinhart RMG. Nat Neurosci. 2022 Sep;25(9):1237-1246. doi: 10.1038/s41593-022-01132-3. Epub 2022 Aug 22. PMID: 35995877.
Funding
NIH’s National Institute on Aging (NIA) and National Institute of Mental Health (NIMH).


