Neural signature predicts antidepressant response
February 25, 2020
Neural signature predicts antidepressant response
At a Glance
- Researchers identified specific patterns of brain activity that predict whether someone with depression is likely to respond to a common antidepressant.
- The findings demonstrate the potential of machine learning to advance personalized treatment for depression.
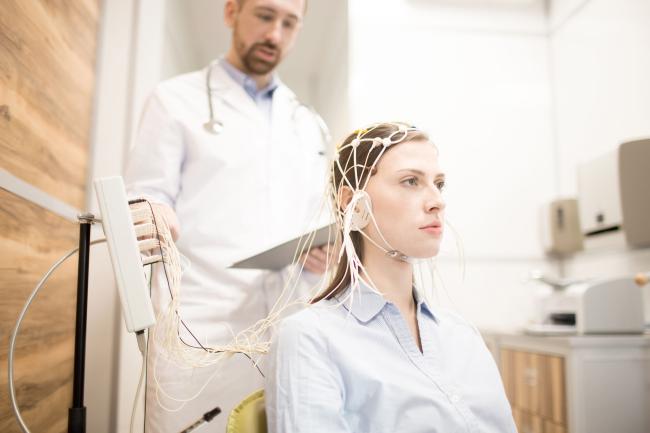
Major depression is a common but serious mood disorder. It affects an estimated 7% of adults in the U.S. Symptoms can vary, but often include persistent sadness and feelings of hopelessness. Treatment for depression usually involves psychotherapy, medication, or a combination. There is no one-size-fits-all approach to treating depression. Finding an effective treatment often requires trial and error.
Researchers set out to identify a pattern of brain activity that could predict the response to antidepressant treatment. The team, led by Dr. Amit Etkin of Stanford University and Dr. Madhukar H. Trivedi at the University of Texas Southwestern Medical Center, was funded in part by NIH’s National Institute of Mental Health (NIMH). Findings appeared in Nature Biotechnology on February 10, 2020.
Previous studies suggested that certain types of brain activity might predict if someone will respond to antidepressants. These studies used electroencephalography, or EEG, a test that records the brain’s electrical activity using electrodes attached to the scalp.
In the current study, the team developed a sophisticated machine learning algorithm to analyze EEG data and predict individual treatment response. Machine learning is a form of artificial intelligence. Researchers input data, enabling the computer to “learn” and create a statistical model to predict outcomes. The team call their algorithm SELSER (for Sparse EEG Latent SpacE Regression).
The researchers used SELSER to analyze data from a clinical trial of the commonly prescribed antidepressant sertraline. In the trial, about 300 participants with depression were randomly assigned to receive either sertraline or an inactive placebo for eight weeks. By applying the SELSER algorithm to the participants’ pre-treatment EEG data, the system learned which EEG patterns were associated with the response to sertraline.
The system found that predictions could be based on the pattern of a specific type of brain signal, known as alpha waves, recorded while participants’ eyes were open.
The researchers next tested whether this neural “signature” they identified could predict treatment response in other data sets of depressed patients. The SELSER model reliably predicted participants' depressive symptoms after treatment. It outperformed other models that used either EEG data or other characteristics, such as symptom severity and demographic information.
Using SELSER, the researchers could also predict which patients would respond to transcranial magnetic stimulation (TMS), a treatment for depression involving non-invasive brain stimulation. Patients predicted to show little improvement with sertraline were more likely to respond to TMS (used in combination with psychotherapy).
These findings highlight the potential for machine learning to advance a personalized approach to treating depression.
"While work remains before the findings in our study are ready for routine clinical use, the fact that EEG is a low-cost and accessible tool makes the translation from research to clinical practice more possible in the near term,” says Etkin.
Related Links
- Predicting the Usefulness of Antidepressants
- Depression Screening and Treatment in Adults
- Placebo Effect in Depression Treatment
- Brain Scan May Predict Best Depression Treatment
- Predicting Treatment Response to a Rapid Antidepressant
- Depression


