You are here
May 15, 2018
Mediterranean diet may slow development of Alzheimer’s disease
At a Glance
- Researchers found that eating a Mediterranean diet slows some changes in the brain that may indicate early Alzheimer’s disease.
- The results point to a lifestyle change that could help reduce the risk of this type of age-related dementia.
Alzheimer’s disease is the most common type of dementia that occurs with aging. Experts estimate that more than 5 million Americans are currently living with the disease. But scientists know little about what lifestyle factors might protect people against developing Alzheimer’s disease. They do know that brain changes associated with the disease can occur decades before symptoms are seen.
In previous work, a research team led by Dr. Lisa Mosconi from Weill Cornell Medicine found differences in brain imaging scans between people who reported eating a Mediterranean diet and those who ate a standard Western diet. A Mediterranean diet is high in foods such as fruits, vegetables, and lean protein. In contrast, a standard Western diet contains an excess of red meat, saturated fats, and refined sugar. The differences that the research team found may signal early Alzheimer’s disease.
In a new study, Mosconi and her colleagues measured changes in brains over time. They performed baseline brain imaging in 34 people who ate a Mediterranean diet and 36 people who ate a Western diet. The volunteers ranged in age from 30 to 60 and showed no symptoms of dementia when the study began. The researchers then repeated the scans at least two years later. The study was supported by NIH’s National Institute on Aging (NIA). Results were published online in Neurology on April 13, 2018.
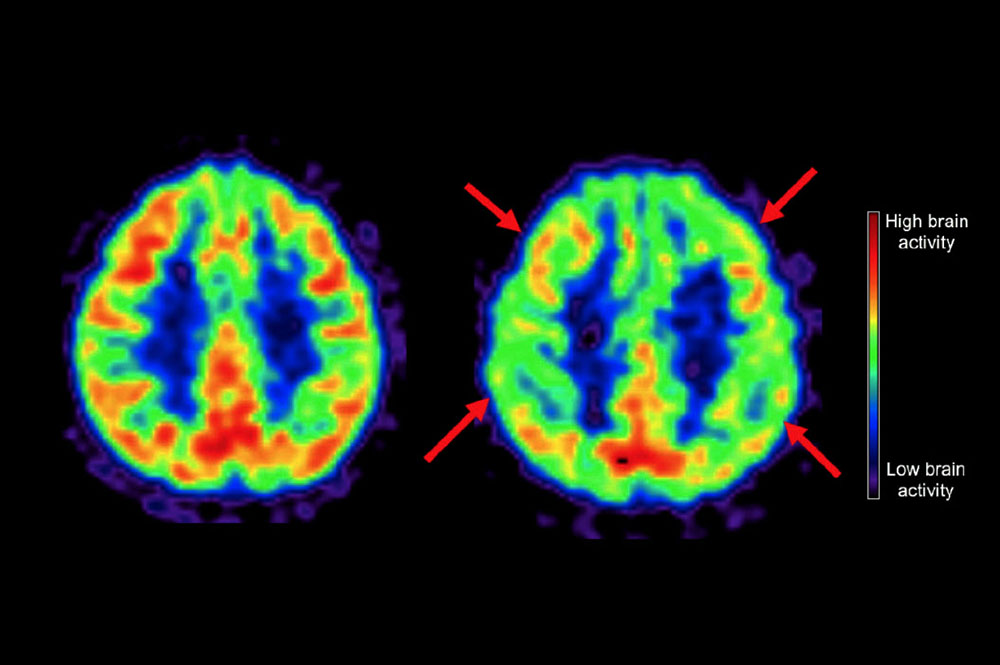
The brain scans taken at the beginning showed that the people who ate a Western diet already had more beta-amyloid deposits than those who ate a Mediterranean diet. Beta-amyloid is a protein known to collect in the brains of people with Alzheimer’s disease. The brains of those who ate a Western diet also showed lower energy use—a sign of brain activity—at the beginning of the study than those who ate a Mediterranean diet. Both these differences suggest the early development of dementia.
In the follow-up scans, people in the Western diet group showed even greater beta-amyloid deposits and reductions in energy use than the Mediterranean diet group. Factors such as age, sex, and a gene linked to Alzheimer’s risk didn’t account for the differences.
“We’re seeing these changes only in parts of the brain specifically affected by Alzheimer’s, and in relatively young adults,” Mosconi says. “It all points to the way we eat putting us at risk for Alzheimer’s down the line. If your diet isn’t balanced, you really need to make an effort to fix it, if not for your body, then for your brain.”
The researchers estimate that there may be as much as a three-and-a-half-year delay in progression of Alzheimer’s disease in people who have eaten a Mediterranean diet for many years, rather than a standard Western diet. Research that involves larger and more diverse groups of people over longer periods of time is needed to confirm these findings. More work is also needed to understand exactly how a Mediterranean diet may protect people from harmful brain changes.
—by Sharon Reynolds
Related Links
- Compound Repairs Features of Alzheimer’s Disease in Mice
- Alzheimer’s Protein May Have Natural Antibiotic Role
- New Genes Tied to Alzheimer’s Disease
- Dealing with Dementia
- Alzheimer’s Disease Fact Sheet
- Frequently Asked Questions About Alzheimer's Disease
References: Mediterranean diet and 3-year Alzheimer brain biomarker changes in middle-aged adults. Berti V, Walters M, Sterling J, Quinn CG, Logue M, Andrews R, Matthews DC, Osorio RS, Pupi A, Vallabhajosula S, Isaacson RS, de Leon MJ, Mosconi L. Neurology. 2018 Apr 13. pii: 10.1212/WNL.0000000000005527. doi: 10.1212/WNL.0000000000005527. [Epub ahead of print] PMID: 29653991.
Funding: NIH’s National Institute on Aging; Weill Cornell Medical College Department of Neurology; and Alzheimer’s Prevention Clinic, Weill Cornell Memory Disorders Program.